Baby constantly drooling: Drooling and Your Baby – HealthyChildren.org
What to Know About Excessive Drooling in Children
Written by Sonia Findlay
- What Is Sialorrhea?
- What Are the Causes of Sialorrhea?
- What Are the Symptoms of Sialorrhea?
- How Is Sialorrhea Diagnosed?
- How Is Sialorrhea Treated?
- When Should You Be Worried About Drooling?
- More
Drooling is common in children between the ages of 15 and 19 months. But after the age of 4, excessive drooling can point to an underlying condition. Sialorrhea, also known as hypersalivation, is usually present in children with neurological or anatomical abnormalities. If you’re worried your child has sialorrhea, here’s what you need to know about the causes, symptoms, and treatments.
Sialorrhea is excessive oral secretion, or drooling. Children usually produce up to 1.5 liters of saliva per day, but children with hypersalivation may produce up to 5 liters. This condition may also happen in children who produce an average amount of saliva but can’t swallow properly.
There are two types of sialorrhea:
Anterior sialorrhea. Anterior sialorrhea is what is commonly referred to as drooling. The excess saliva spills onto the child’s face and, if left unchecked, their clothes. This can cause issues with skin care and cleanliness. Because of this, they may also have issues with socializing.
Posterior sialorrhea. Posterior sialorrhea is when the saliva spills down the child’s airway instead of being swallowed. This form of hypersalivation leads to chronic lung irritation, which can cause other health issues.
Children with sialorrhea typically have a combination of anterior and posterior sialorrhea.
Sialorrhea in children is often caused by existing underlying diseases. Conditions that affect the brain can cause reduced muscle control, especially around the mouth and throat. This leads to difficulty swallowing saliva and results in excessive drooling.
Excessive oral secretions are common in children who are born with cerebral palsy, which is a condition that affects the brain’s ability to move muscles.
Other conditions that affect motor control of the mouth and throat include stroke, traumatic brain injuries, and abnormalities in brain development. The severity of the sialorrhea normally depends on the severity of the underlying disease. For example, if the brain injury does not worsen over time, the excessive drooling shouldn’t either.
Sialorrhea also happens in children with anatomical abnormalities that lead to physical difficulties swallowing. Hypersalivation causes may include:
- A large tongue
- A malformed jaw
- A malformed throat
- Orthodontic issues
- Clefts in the lip, palate, or larynx
Excessive drooling can also be caused by the child’s body producing too much saliva or mucus rather than their inability to swallow. This can happen as a result of other neurological or respiratory conditions or as a side effect of certain medications.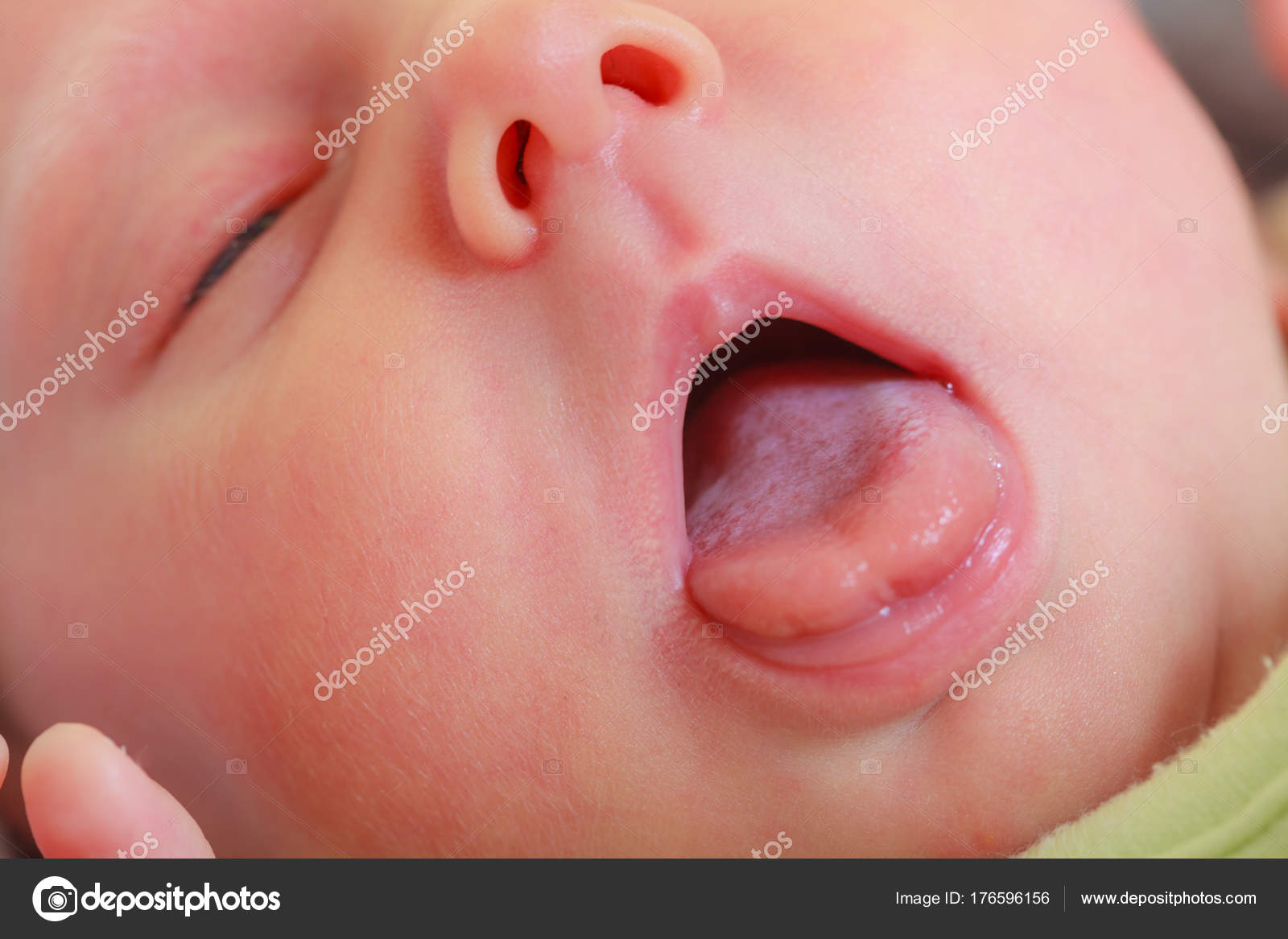
Hypersalivation symptoms depend on whether the saliva is being drooled onto the child’s face or spilling into their airway.
Children with anterior sialorrhea have visible drooling that is usually accompanied by wet clothing. If the drooling is severe, the child’s bed sheets may also be wet after sleeping.
Constant drooling can lead to facial rashes and the breakdown of skin around the mouth and chin. This can cause some irritation and soreness.
Children with sialorrhea may also have mild dehydration, difficulties with speech, and feeding issues as a side effect of constant drooling.
Children with posterior sialorrhea may have more serious symptoms due to chronic lung irritation and a blocked airway. Symptoms can include:
- Choking
- Coughing
- Gagging
- Vomiting
- Congestion
- Breathing difficulty
- Aspiration
Aspiration, which is breathing in non-air substances, is especially dangerous as it can lead to pneumonia.
Healthcare professionals can diagnose anterior sialorrhea by observation. Excessive drooling is an easily identifiable, visible symptom. Posterior sialorrhea diagnosis may need additional tests.
To identify posterior sialorrhea, doctors can use special equipment and procedures to examine the child’s throat as well as their swallowing and speech functions. This often involves the use of videofluoroscopy, which is a specific type of x-ray used to assess swallowing.
Sialorrhea treatments include oral medications, botox injections, surgical procedures, and oral motor training.
Oral medications. Doctors may prescribe oral medications to reduce saliva production or ease the child’s airway. The side effects of this medication may be uncomfortable or lead to other health complications. Anticholinergic medications, which are used to ease airways, usually cause dry mouth and constipation.
More serious side effects include fever and thicker secretions, which can cause further respiratory issues.
Botox injections. Studies show that botulinum toxin, or botox, can safely treat sialorrhea in children. Doctors can reduce saliva production for around 4 months by injecting botox into the salivary glands.
Surgical procedures. There are many surgeries for the treatment of sialorrhea. Usually, they involve removing or disconnecting some salivary glands from the child’s mouth. By permanently reducing saliva production, some surgeries can curatively treat excessive drooling.
Oral motor training. Children who drool due to physical malformations should consider doing oral motor training, such as speech or swallowing therapy, if they can. This can help them learn how to swallow properly and reduce the amount of excess drool.
Mild cases of sialorrhea may not need aggressive treatment. You can manage drooling by using bibs or other cloths to absorb excess oral secretion.
Drooling often happens in young children who haven’t yet developed the proper motor control or awareness to swallow their saliva. But, by the age of four, children should be able to control their drooling habits. After this age, excessive drooling may be a sign of an underlying condition. If you’re unaware that your child has any existing conditions, you should seek additional advice from your doctor.
Excessive drooling usually doesn’t cause serious medical problems, especially if it’s anterior sialorrhea. But if sialorrhea has started to affect your child’s quality of life, it may be worthwhile to seek more advanced treatment from your doctor.
You should also keep in mind that if the onset of sialorrhea is sudden, excessive drooling may be a sign of a throat infection or that your child has swallowed an object.
In all cases, it’s important to take your child to a doctor to get the correct diagnosis and treatment.
Top Picks
What to Know About Excessive Drooling in Children
Written by Sonia Findlay
- What Is Sialorrhea?
- What Are the Causes of Sialorrhea?
- What Are the Symptoms of Sialorrhea?
- How Is Sialorrhea Diagnosed?
- How Is Sialorrhea Treated?
- When Should You Be Worried About Drooling?
- More
Drooling is common in children between the ages of 15 and 19 months. But after the age of 4, excessive drooling can point to an underlying condition.
Sialorrhea is excessive oral secretion, or drooling. Children usually produce up to 1.5 liters of saliva per day, but children with hypersalivation may produce up to 5 liters. This condition may also happen in children who produce an average amount of saliva but can’t swallow properly.
There are two types of sialorrhea:
Anterior sialorrhea. Anterior sialorrhea is what is commonly referred to as drooling. The excess saliva spills onto the child’s face and, if left unchecked, their clothes. This can cause issues with skin care and cleanliness. Because of this, they may also have issues with socializing.
Posterior sialorrhea. Posterior sialorrhea is when the saliva spills down the child’s airway instead of being swallowed.
Children with sialorrhea typically have a combination of anterior and posterior sialorrhea.
Sialorrhea in children is often caused by existing underlying diseases. Conditions that affect the brain can cause reduced muscle control, especially around the mouth and throat. This leads to difficulty swallowing saliva and results in excessive drooling.
Excessive oral secretions are common in children who are born with cerebral palsy, which is a condition that affects the brain’s ability to move muscles. Some studies suggest that up to 58% of children with cerebral palsy also have sialorrhea.
Other conditions that affect motor control of the mouth and throat include stroke, traumatic brain injuries, and abnormalities in brain development. The severity of the sialorrhea normally depends on the severity of the underlying disease. For example, if the brain injury does not worsen over time, the excessive drooling shouldn’t either.
Sialorrhea also happens in children with anatomical abnormalities that lead to physical difficulties swallowing. Hypersalivation causes may include:
- A large tongue
- A malformed jaw
- A malformed throat
- Orthodontic issues
- Clefts in the lip, palate, or larynx
Excessive drooling can also be caused by the child’s body producing too much saliva or mucus rather than their inability to swallow. This can happen as a result of other neurological or respiratory conditions or as a side effect of certain medications.
Hypersalivation symptoms depend on whether the saliva is being drooled onto the child’s face or spilling into their airway.
Children with anterior sialorrhea have visible drooling that is usually accompanied by wet clothing. If the drooling is severe, the child’s bed sheets may also be wet after sleeping.
Constant drooling can lead to facial rashes and the breakdown of skin around the mouth and chin. This can cause some irritation and soreness.
Children with sialorrhea may also have mild dehydration, difficulties with speech, and feeding issues as a side effect of constant drooling.
Children with posterior sialorrhea may have more serious symptoms due to chronic lung irritation and a blocked airway. Symptoms can include:
- Choking
- Coughing
- Gagging
- Vomiting
- Congestion
- Breathing difficulty
- Aspiration
Aspiration, which is breathing in non-air substances, is especially dangerous as it can lead to pneumonia.
Healthcare professionals can diagnose anterior sialorrhea by observation. Excessive drooling is an easily identifiable, visible symptom. Posterior sialorrhea diagnosis may need additional tests.
To identify posterior sialorrhea, doctors can use special equipment and procedures to examine the child’s throat as well as their swallowing and speech functions. This often involves the use of videofluoroscopy, which is a specific type of x-ray used to assess swallowing.
Sialorrhea treatments include oral medications, botox injections, surgical procedures, and oral motor training.
Oral medications. Doctors may prescribe oral medications to reduce saliva production or ease the child’s airway. The side effects of this medication may be uncomfortable or lead to other health complications. Anticholinergic medications, which are used to ease airways, usually cause dry mouth and constipation.
More serious side effects include fever and thicker secretions, which can cause further respiratory issues. Because of this, medication may only be appropriate for serious cases of hypersalivation in children.
Botox injections. Studies show that botulinum toxin, or botox, can safely treat sialorrhea in children. Doctors can reduce saliva production for around 4 months by injecting botox into the salivary glands.
Surgical procedures. There are many surgeries for the treatment of sialorrhea. Usually, they involve removing or disconnecting some salivary glands from the child’s mouth.
Oral motor training. Children who drool due to physical malformations should consider doing oral motor training, such as speech or swallowing therapy, if they can. This can help them learn how to swallow properly and reduce the amount of excess drool.
Mild cases of sialorrhea may not need aggressive treatment. You can manage drooling by using bibs or other cloths to absorb excess oral secretion. Additionally, you can use barrier creams around the mouth and chin to help prevent skin irritation.
Drooling often happens in young children who haven’t yet developed the proper motor control or awareness to swallow their saliva. But, by the age of four, children should be able to control their drooling habits. After this age, excessive drooling may be a sign of an underlying condition. If you’re unaware that your child has any existing conditions, you should seek additional advice from your doctor.
Excessive drooling usually doesn’t cause serious medical problems, especially if it’s anterior sialorrhea. But if sialorrhea has started to affect your child’s quality of life, it may be worthwhile to seek more advanced treatment from your doctor.
You should also keep in mind that if the onset of sialorrhea is sudden, excessive drooling may be a sign of a throat infection or that your child has swallowed an object.
In all cases, it’s important to take your child to a doctor to get the correct diagnosis and treatment.
Top Picks
|
During the “baby boom” period, I often have to listen to young mothers who enthusiastically talk about their beloved children. Let’s figure it out together: The formation of a milk bite is of great importance, since the further development of the entire maxillofacial system depends on it. Therefore, maintaining a healthy condition of milk teeth is an important task. However, we will talk about this in detail in the next article. So, milk bite consists of twenty teeth. Usually, by 6-8 months of a child’s life, the central incisors of the lower jaw (1 or 2 teeth) erupt. They are followed by the central incisors of the mandible. At 8-12 months, lateral incisors appear first on the lower, then on the upper jaw. The first molars usually appear by 12-16 months, at 16-20 months – fangs, and, finally, by 20-30 months – the last, second molars. Some parents are concerned about the asymmetric placement of baby teeth. It is believed that the process of teething is difficult for both the baby and the parents: The child becomes capricious, often cries, “drools”, pulls everything that is tucked under the arm into his mouth, he has a fever and problems with the intestines … Here it is worth making a few digressions: Firstly: from the age of four months, children have increased salinity, i.e. salivation. It seems to parents that the first long-awaited tooth is about to erupt, but a month or two passes, and nothing happens. Do not panic: often the interval between the start of active work of the salivary glands and the appearance of the first teeth is two to three months. Secondly: the baby puts everything in his mouth not only because he is teething, but also because in certain months of his life tasting various objects for taste and hardness is one of the ways of learning about the world around him. And thirdly, it used to be believed that due to teething, babies have problems with the intestines, as well as a rise in temperature. But modern scientists have come to the conclusion that these problems are not directly related to the first teeth: just during teething, the child’s general immunity decreases, and he becomes more susceptible to various bacteria and infections. Therefore, having discovered such signs, it is better to immediately consult a pediatrician to exclude the possibility of developing infectious diseases. Finally, not all families experience the first teething of a baby as a nightmare. Some children tolerate these changes quite calmly and do not cause much concern to parents. If your baby is still very unwell and has difficulty sleeping due to pain, talk to your doctor about an over-the-counter pain reliever made specifically for babies, and check with your doctor about dosage. Now let’s talk about a problem that a close friend of mine faced recently: her son didn’t have a single tooth by 12 months. Naturally, the son was taken to a pediatric dentist. The dentist issued a sacramental phrase: “Have you ever seen children who never erupted a single tooth? Here I am, no. Go home and wait.” ))) Now the child is almost three years old, all the set teeth are in place, and mom really shouldn’t have worried. But, since the doctor apparently believed that brevity is the sister of talent, I will try to expand on this topic. In the world, of course, there are cases of complete absence of teeth (in professional language – adentia), but they are extremely (!) Rare. But cases of later eruption have become more frequent. (There are a lot of reasons – from poor ecology, lack of vitamins and genetic heredity, to an elementary “personal” program laid down by nature) By the way, in such cases they say about late erupted teeth: they will grow later – they will last longer. Also, cases of partial absence of teeth and their rudiments have become more frequent, which may be associated with a change in nutrition: human food has become softer, it no longer needs to be chewed so hard, and little-used teeth simply do not grow. Most often these are the lateral upper incisors, the second upper or lower premolars. To confirm the absence of the germ, it is necessary to take a panoramic x-ray (orthopantogram) when the baby is about 7 years old, especially if relatives or parents already had similar features. Early diagnosis will help find a solution to the problem: it can be a bridge prosthesis or implantation, which is carried out at a more mature age, when the maxillofacial skeleton is sufficiently formed. In any case, if you are worried that the baby has not yet erupted its first tooth, dentists advise you to wait until 1.5 – 2 years, and then take it to a specialist, having previously made an orthopantogram. Do not forget that your child is a bright individual with his own development program, so do not panic if he has his own pace of life, different from others. |
Reasons why a child worries parents
10.06.2022
The baby changes from week to week. However, sometimes new changes in a child’s behavior are worrisome, especially when the child is crying, snoring, or drooling heavily. Although they are rarely a precursor to symptoms, sometimes they cannot be ruled out.
What to do if the baby cries, snores, screams in the bath, makes strange sounds puts hands in ‘s mouth and drools a lot – what behavior might bother an infant? These are the most common questions that concern young mothers.
The child cries when bathing
It seems quite likely that the reason for crying and not wanting to bathe is too hot water. So it is worth immersing the child in slightly cooler water, with a temperature of about 36 ° C.
Sometimes children feel bad when they are immersed in water too quickly. Crying can be triggered by sudden changes in body position and temperature. Some babies just don’t like wet contact. The solution may be to soak the child wrapped in a diaper and only after immersion unroll it, but leave it in the water.
Perhaps if you pour more water, your child will be comfortable. However, you need to be careful, because then the child is more difficult to control, especially if he fidgets. An inflatable bath ring can also be useful. The child is almost completely immersed in water, only the head sticks out of the water (you need to hold it with one hand). The baby leans on the walls of the tub with its back , bottom and legs.
Wheezing and snoring baby
If your baby snores and wheezes outside of sleep, he may have an infection. Airway inflammation causes edema tissues.
Sometimes the air in a child’s bedroom is too dry. Then you can hang a container of water in the room and pour salt water or saline solution on the child. However, if snoring is present constantly, during wakefulness and sleep, especially in the supine position , and the child is healthy, laryngeal weakness is likely to be the cause. The child gets the impression that each breath is an effort for him. The narrowing of the larynx, caused by the weakness of its cartilage and ligamentous apparatus, is to blame.
During inhalation, the flaccid cartilage of the larynx is slightly destroyed, narrowing it, making it difficult to inhale. This condition usually goes away with age. If your child is developing correctly and gaining weight well, there is nothing left but to wait until the larynx matures. This usually happens within a few months.
Baby drooling
If your baby puts his hands in mouth and drools, it’s worth checking the gums.
If the gums do not bother, the salivation is probably caused by a surge in the maturation of the digestive system, namely the salivary glands. It remains to wait until their work will improve. After 2-3 weeks, salivation will become a little less abundant.
Cleaning the ears with cotton swabs
Do not insert cotton swabs into the ear . Thus, it is possible not only to cut the epithelium, increase the production of earwax, but also damage the structures located there. Earwax is needed to protect the ear canal and get rid of debris from the ear . If your child has earwax, it is enough to rinse the auricle and the visible entrance to the ear canal. It is also worth paying attention to the area behind the nasal concha, because children often accumulate food debris there.
Spots on the child’s neck
If you are worried about visible spots on the neck of the child, then do not panic. The spots will not fade, but will fade a little and be covered with hair. In the future, they won’t be visible at all.
These are hemangiomas, that is, foci of dilated small blood vessels . They become more noticeable when the child is exercising or is exposed to high temperatures, because then the vessels dilate and more blood enters them. They turn pale from the cold and do not pose a threat to the health of the child.
Finger in child’s mouth
Sticking thumb in mouth is usually due to fatigue, need for closeness or anxiety. You must memorize the circumstances in which the finger hits mouth baby. If this is the effect of overwork, it’s time to be quiet with the baby and take a nap. Conversely, if it happens when your baby is restless, crying, or seems tense, cuddling, carrying, rocking, or relaxing stimuli and sensations may help.







 An exciting topic, according to my observation, is the concern of parents about the first teeth of a child: what time should they erupt, how to help the baby during this period and how many teeth should erupt in the end?
An exciting topic, according to my observation, is the concern of parents about the first teeth of a child: what time should they erupt, how to help the baby during this period and how many teeth should erupt in the end? 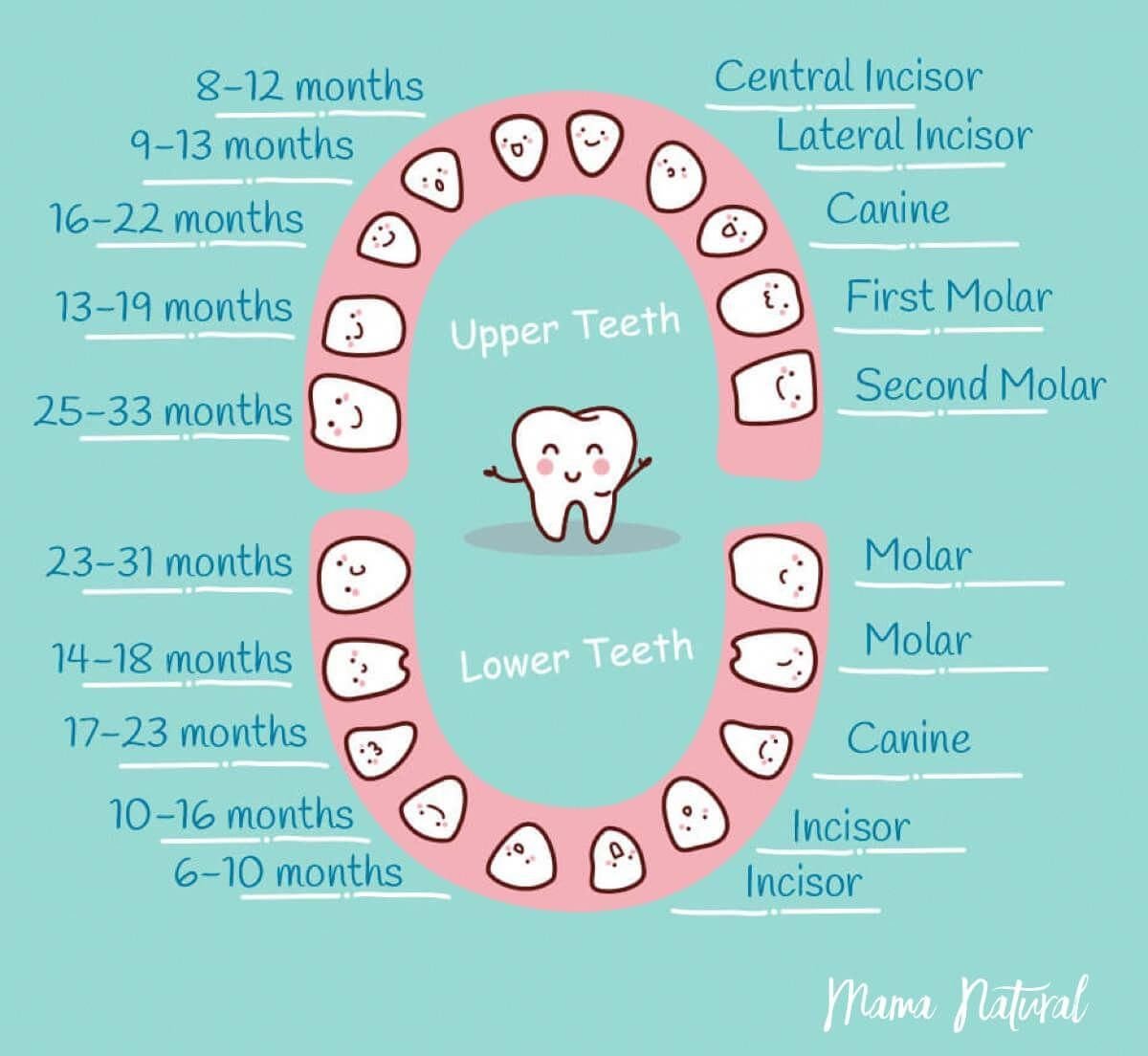 However, this is not considered a disease. The fact is that, usually, after eruption of 16 teeth, as a result of chewing food, milk teeth “grind” and fall into place.
However, this is not considered a disease. The fact is that, usually, after eruption of 16 teeth, as a result of chewing food, milk teeth “grind” and fall into place.  If the gums are swollen and reddened, and the child is naughty, use special anesthetic gels for children (for many mothers they have become a real real salvation) and buy a special rubber ring for gum massage for the baby. It can be whole, or filled with cool water, which has an additional calming effect.
If the gums are swollen and reddened, and the child is naughty, use special anesthetic gels for children (for many mothers they have become a real real salvation) and buy a special rubber ring for gum massage for the baby. It can be whole, or filled with cool water, which has an additional calming effect. 
 )))
)))  The main thing is to let him know that he is special, and not dryly “not like everyone else.” And then he will smile. Not only to show his first teeth, but also because he is truly happy.
The main thing is to let him know that he is special, and not dryly “not like everyone else.” And then he will smile. Not only to show his first teeth, but also because he is truly happy. 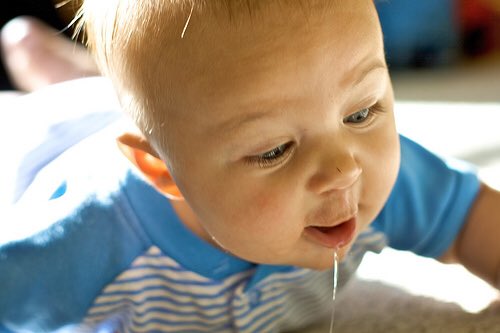
 All the founders, except for Katz, still work in the office-Wachtell and Lipton as partners, and Rosen as Of Counsel. Their first-year associates are given a starting salary of $165,000, in addition to a whopping bonus that ranges from 50-100% of their entire salary.
All the founders, except for Katz, still work in the office-Wachtell and Lipton as partners, and Rosen as Of Counsel. Their first-year associates are given a starting salary of $165,000, in addition to a whopping bonus that ranges from 50-100% of their entire salary. It was the first law firm to ever reach $1 billion in annual revenue. Skadden’s starting salary is $160,000.
It was the first law firm to ever reach $1 billion in annual revenue. Skadden’s starting salary is $160,000. Cleary Gottlieb has awarded its foreign lawyers equal partnership in the firm, gaining a strong advantage in its international presence. The starting salary is $160,000.
Cleary Gottlieb has awarded its foreign lawyers equal partnership in the firm, gaining a strong advantage in its international presence. The starting salary is $160,000. But remember, there are hundreds of amazing firms that are changing the world day by day.
But remember, there are hundreds of amazing firms that are changing the world day by day.
 47
47 74
74 73
73 81
81 24
24
 61
61 47
47 95
95 39
39 51
51 49
49 38
38 9
9 9
9 9
9 8
8 Compared to the industry average of $116,226 per year, the average annual salary at WLRK is $116,904, which is 0.58% higher.
Compared to the industry average of $116,226 per year, the average annual salary at WLRK is $116,904, which is 0.58% higher.

 Nussbaum, who gave a lecture to students of the Higher School of Economics on the role of litigation in American M&A practice, explained how one of the brightest companies in the American legal market is organized and why it is important for a novice lawyer to work in court.
Nussbaum, who gave a lecture to students of the Higher School of Economics on the role of litigation in American M&A practice, explained how one of the brightest companies in the American legal market is organized and why it is important for a novice lawyer to work in court.  Lawyers are known for taking on hard work, the Vault explained. However, there can be no easy job for such a company: it specializes in large and complex transactions, including a $ 50 billion deal for the purchase of Merrill Lynch by Bank of America. However, the firm is unlike its competitors, said Andrew Nussbaum, a partner in the company’s corporate practice. The reason is the professionalism of partners; for example, Nussbaum, who worked for Wachtell, Lipton, Rosen & Katz for many years, previously served as an assistant to the most prominent judges of the US Armed Forces, often taking diametrically opposed positions in disputes – Ruth Ginzburg and Antonina Scalia. But not only – it is also a special attitude to the matter.
Lawyers are known for taking on hard work, the Vault explained. However, there can be no easy job for such a company: it specializes in large and complex transactions, including a $ 50 billion deal for the purchase of Merrill Lynch by Bank of America. However, the firm is unlike its competitors, said Andrew Nussbaum, a partner in the company’s corporate practice. The reason is the professionalism of partners; for example, Nussbaum, who worked for Wachtell, Lipton, Rosen & Katz for many years, previously served as an assistant to the most prominent judges of the US Armed Forces, often taking diametrically opposed positions in disputes – Ruth Ginzburg and Antonina Scalia. But not only – it is also a special attitude to the matter. 
 This is less effective,” says Nussbaum. In the company, in fact, they apply the principle of “sink or swim” – the partner gives the lawyer the same job that he is busy with and expects a colleague to figure it out.
This is less effective,” says Nussbaum. In the company, in fact, they apply the principle of “sink or swim” – the partner gives the lawyer the same job that he is busy with and expects a colleague to figure it out. 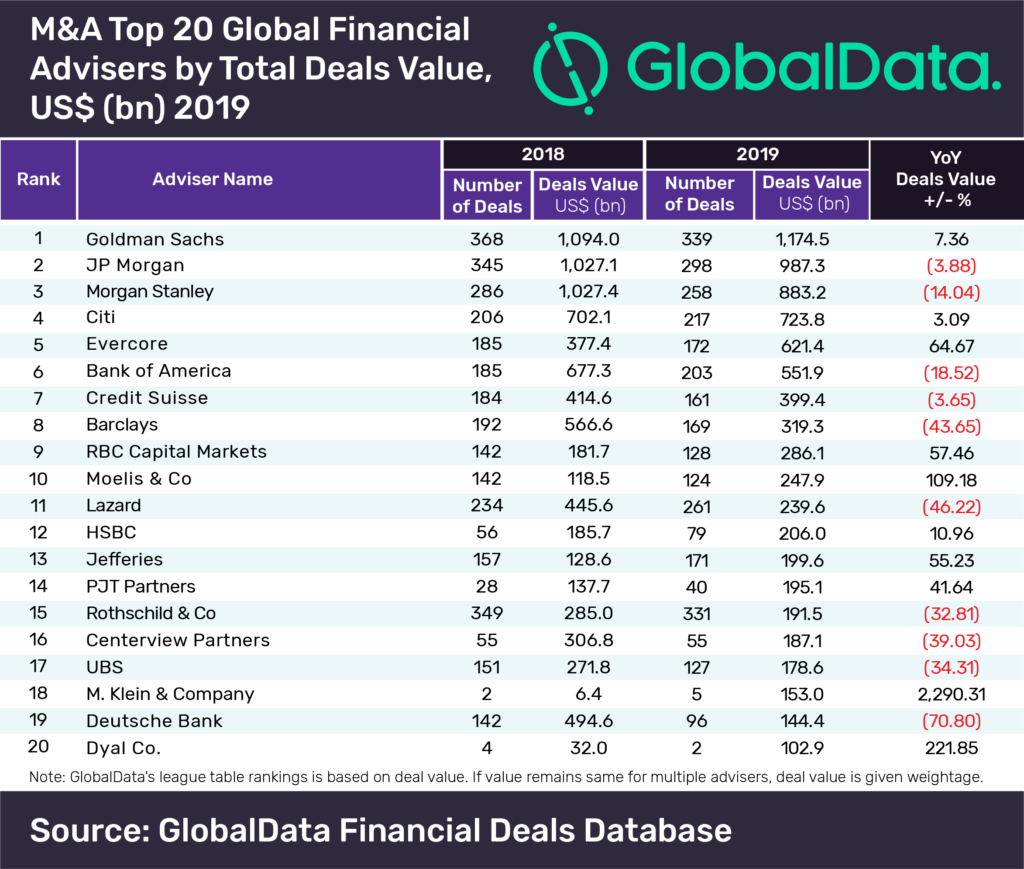 “In England, there were special desks for partners. They were quite long. The partner sat on one side, and the young employees sat on the other. The way of learning law for young barristers and solicitors was to observe what the partner was doing and then repeat the actions for him. In theory, a young lawyer learned in this way, turned into a qualified specialist, because he was in direct contact with professionals who did a very high quality job,” Nussbaum said.
“In England, there were special desks for partners. They were quite long. The partner sat on one side, and the young employees sat on the other. The way of learning law for young barristers and solicitors was to observe what the partner was doing and then repeat the actions for him. In theory, a young lawyer learned in this way, turned into a qualified specialist, because he was in direct contact with professionals who did a very high quality job,” Nussbaum said. 
 Usually clients are satisfied and agree, but sometimes they can say that they want to pay less or, conversely, more, because they really liked the way we work. It must be said that in litigation we sometimes still use billing in addition to the success fee, but this depends on the nature of the dispute.”
Usually clients are satisfied and agree, but sometimes they can say that they want to pay less or, conversely, more, because they really liked the way we work. It must be said that in litigation we sometimes still use billing in addition to the success fee, but this depends on the nature of the dispute.” 
 No, seriously, we have a really terrible governance system. With one exception – it suits us perfectly,” Nussbaum ironically. The system, he says, is highly informal: “Two partners run the firm, which is a terrible job because they have a lot of decisions to make, and most of us are very happy that someone else does it: sometimes someone needs to be fired, decide how to dispose of office space, and so on. In general, a whole bunch of cases, and, you know, I would rather deal with transactions.”
No, seriously, we have a really terrible governance system. With one exception – it suits us perfectly,” Nussbaum ironically. The system, he says, is highly informal: “Two partners run the firm, which is a terrible job because they have a lot of decisions to make, and most of us are very happy that someone else does it: sometimes someone needs to be fired, decide how to dispose of office space, and so on. In general, a whole bunch of cases, and, you know, I would rather deal with transactions.”  This is Wachtell’s model of work, as partners need to be involved in the project and communicate directly with customers.
This is Wachtell’s model of work, as partners need to be involved in the project and communicate directly with customers.  not sure <...> better call so-and-so. We know they’re the perfect fit for you.”0003
not sure <...> better call so-and-so. We know they’re the perfect fit for you.”0003 
 “Look at our website! It’s terrible! It’s immediately clear that the company does not have a single marketer,” says Nussbaum. However, the company does not need them, he is sure.
“Look at our website! It’s terrible! It’s immediately clear that the company does not have a single marketer,” says Nussbaum. However, the company does not need them, he is sure.  He is now the CEO of Naspers and the owner of a fortune estimated by Forbes at $1.67 billion
He is now the CEO of Naspers and the owner of a fortune estimated by Forbes at $1.67 billion  “It was a great revelation.”
“It was a great revelation.”  “Cellular telephony has radically changed society. Imagine how plumbers worked in the 1990s: they went to one job, returned to the office, received instructions, went to another,” Becker explained. “Now imagine how he lives now: you are always on the road and you don’t see the office.”
“Cellular telephony has radically changed society. Imagine how plumbers worked in the 1990s: they went to one job, returned to the office, received instructions, went to another,” Becker explained. “Now imagine how he lives now: you are always on the road and you don’t see the office.”  An example of this is our investment in Chinese business in 1997 year. All of them turned out to be failures. On one of them, a Beijing Internet provider, we lost $ 80 million – all our money, ”Becker recalled.
An example of this is our investment in Chinese business in 1997 year. All of them turned out to be failures. On one of them, a Beijing Internet provider, we lost $ 80 million – all our money, ”Becker recalled.  Now the capitalization of Tencent is $192 billion. The Chinese company is successfully developing businesses in the markets of online media, e-commerce, social networks, social services, mobile applications and online games. The messenger she initially worked on was called QQ, and at the end of 2015 it was used by 853 million people a month (plus 5% compared to last year). “They [the Chinese] came from nowhere at 1990s, and now they are the second, after the USA, the most dynamic market in the world. Big players like Baidoo, Tencent and Alibaba are well on their feet,” Becker said.
Now the capitalization of Tencent is $192 billion. The Chinese company is successfully developing businesses in the markets of online media, e-commerce, social networks, social services, mobile applications and online games. The messenger she initially worked on was called QQ, and at the end of 2015 it was used by 853 million people a month (plus 5% compared to last year). “They [the Chinese] came from nowhere at 1990s, and now they are the second, after the USA, the most dynamic market in the world. Big players like Baidoo, Tencent and Alibaba are well on their feet,” Becker said.  6% through its holding company MIH, another 7.4% belonged to Tencent. As of March 31, the capitalization of Mail.Ru Group was $4.8 billion. In October 2015, Naspers announced its intention to become the largest shareholder of the largest ad site in Russia, Avito, by buying out the shares of several shareholders for $1.2 billion: as a result, Naspers’ share in Avito should grow from 17.4 to 67.9%. According to TNS Russia, in February 2016 Avito was the eighth most popular site in Runet with a monthly audience of 25.7 million people.
6% through its holding company MIH, another 7.4% belonged to Tencent. As of March 31, the capitalization of Mail.Ru Group was $4.8 billion. In October 2015, Naspers announced its intention to become the largest shareholder of the largest ad site in Russia, Avito, by buying out the shares of several shareholders for $1.2 billion: as a result, Naspers’ share in Avito should grow from 17.4 to 67.9%. According to TNS Russia, in February 2016 Avito was the eighth most popular site in Runet with a monthly audience of 25.7 million people.  In April 2015, he returned to the company as non-executive chairman of the board of directors. A month later, in a conversation with Bloomberg, Becker explained that the company’s challenge was “to find countries where there is still room for growth, as many good opportunities have already been missed.” He wants to prove that Naspers is not just a giant venture capital fund built entirely on a single Chinese investment.0003
In April 2015, he returned to the company as non-executive chairman of the board of directors. A month later, in a conversation with Bloomberg, Becker explained that the company’s challenge was “to find countries where there is still room for growth, as many good opportunities have already been missed.” He wants to prove that Naspers is not just a giant venture capital fund built entirely on a single Chinese investment.0003 


 These small settings also allow educators to tailor learning programs to suit children’s individual needs while offering unique, diverse experiences in an enriching home learning environment.
These small settings also allow educators to tailor learning programs to suit children’s individual needs while offering unique, diverse experiences in an enriching home learning environment.  Family day care on the other hand can only accommodate a limited number of children who attend altogether.
Family day care on the other hand can only accommodate a limited number of children who attend altogether.


 Parents aren’t left without a back-up plan for child care if their child attends a commercial child care center.
Parents aren’t left without a back-up plan for child care if their child attends a commercial child care center. Kids also take naps and eat meals and snacks with their peers. With infants, each child’s unique schedule is followed to provide a home away from home.
Kids also take naps and eat meals and snacks with their peers. With infants, each child’s unique schedule is followed to provide a home away from home.










 com verified on 06/27/2023
com verified on 06/27/2023 Our teachers are
Our teachers are Reports can also be verified with your local daycare licensing office.
Reports can also be verified with your local daycare licensing office. We will research your concern and make corrections accordingly.
We will research your concern and make corrections accordingly. We will assess
We will assess 02.2017
02.2017 When the gangster dies, his girlfriend Teresa (Janelle Monae) takes care of the boy. As Sharon grows and matures, he realizes that he differs from other guys not only in behavior, but also in sexual orientation.
When the gangster dies, his girlfriend Teresa (Janelle Monae) takes care of the boy. As Sharon grows and matures, he realizes that he differs from other guys not only in behavior, but also in sexual orientation.  When you read Western critics, it seems that Jenkins is the new coming of Christ and that his film is the best thing that has happened in cinema in the last decade.
When you read Western critics, it seems that Jenkins is the new coming of Christ and that his film is the best thing that has happened in cinema in the last decade.  Each of these chapters could and should have been a feature-length film in its own right – especially the first chapter, where a kind-hearted drug dealer enters the boy’s life, and the third chapter, where Sharon musters up the courage to confess her feelings to a former classmate.
Each of these chapters could and should have been a feature-length film in its own right – especially the first chapter, where a kind-hearted drug dealer enters the boy’s life, and the third chapter, where Sharon musters up the courage to confess her feelings to a former classmate. 
 Our students will be expected to reach their fullest potential and our teachers will demonstrate con …
Our students will be expected to reach their fullest potential and our teachers will demonstrate con … Our theme this year is “Common Core Strong” …
Our theme this year is “Common Core Strong” … ..
.. This child care center helps with children in the age range of 0 through 12. The provider also participates in a subsidized child ca …
This child care center helps with children in the age range of 0 through 12. The provider also participates in a subsidized child ca … We offer children a fun and educational curriculum that will help children develop socially while providing a str …
We offer children a fun and educational curriculum that will help children develop socially while providing a str … This child care center helps with children in the age range of 0 through 12. The provider also participates in a …
This child care center helps with children in the age range of 0 through 12. The provider also participates in a … More>>
More>> It was a trip the we will fondly remember forever. Anything and everything that you could want was available for the entire family. We first stayed on beautiful Maui and next ventured to the big Island of Hawaii during our 11 day visit……
It was a trip the we will fondly remember forever. Anything and everything that you could want was available for the entire family. We first stayed on beautiful Maui and next ventured to the big Island of Hawaii during our 11 day visit…… The constant demands of caring for young children can be exhausting, both physically and emotionally, and can take a toll on providers over time. Burnout can negatively impact not only providers, but also the children in their care and the families who depend on them. In this essay, we will explore the causes and effects of provider burnout and discuss strategies for preventing and managing burnout in the daycare industry……..
The constant demands of caring for young children can be exhausting, both physically and emotionally, and can take a toll on providers over time. Burnout can negatively impact not only providers, but also the children in their care and the families who depend on them. In this essay, we will explore the causes and effects of provider burnout and discuss strategies for preventing and managing burnout in the daycare industry…….. 

 It provides detailed explanations of each account, including the 529 College Savings Plan, Coverdell Education Savings Accounts, and Custodial Accounts. The article cites applicable legal authorities and emphasizes the importance of informed decision-making by consulting with legal and financial professionals.
It provides detailed explanations of each account, including the 529 College Savings Plan, Coverdell Education Savings Accounts, and Custodial Accounts. The article cites applicable legal authorities and emphasizes the importance of informed decision-making by consulting with legal and financial professionals. This district’s average testing ranking is 9/10, which is in the top 20% of public schools in New Jersey.
This district’s average testing ranking is 9/10, which is in the top 20% of public schools in New Jersey. The school district revenue/student has stayed relatively flat over four school years.
The school district revenue/student has stayed relatively flat over four school years.
 This district ranks in the top 20% of New Jersey school districts for: Highest overall rank (Top 20%), Highest math proficiency (Top 20%), Highest reading/language arts proficiency (Top 20%), Highest graduation rate (Top 5%) and Largest student body (number of students) (Top 1%)
This district ranks in the top 20% of New Jersey school districts for: Highest overall rank (Top 20%), Highest math proficiency (Top 20%), Highest reading/language arts proficiency (Top 20%), Highest graduation rate (Top 5%) and Largest student body (number of students) (Top 1%)
 Private School
Private School 3 Political career
3 Political career


 Although doctors initially thought the treatment would require her tongue to be removed and she would not be able to speak normally, surgery in 2010 did not greatly affect her speech, and she has since undergone radiation therapy and a laser.
Although doctors initially thought the treatment would require her tongue to be removed and she would not be able to speak normally, surgery in 2010 did not greatly affect her speech, and she has since undergone radiation therapy and a laser.
 Retrieved July 6, 2006.
Retrieved July 6, 2006.
 “New Jersey Daily Briefing; campaign cost $1 million”, The New York Times , 13 March 1996. Retrieved June 22, 2010.
“New Jersey Daily Briefing; campaign cost $1 million”, The New York Times , 13 March 1996. Retrieved June 22, 2010.
 7th District: Allen Holds Senate Seat, The Star-Ledger , November 6, 2007
7th District: Allen Holds Senate Seat, The Star-Ledger , November 6, 2007
 ”
”
 The episode offers a first-hand look at #NJInnovation from Newark-based companies like Audible and AeroFarms.
The episode offers a first-hand look at #NJInnovation from Newark-based companies like Audible and AeroFarms. 

 FirstEnergy is involved in the renovation of Fort Monmouth to improve the electrical grid.
FirstEnergy is involved in the renovation of Fort Monmouth to improve the electrical grid. 
 Labels are everywhere to help kids connect
Labels are everywhere to help kids connect We welcome children ages 5–12 during school break times and make sure they have a
We welcome children ages 5–12 during school break times and make sure they have a
 Being a great educator isn’t enough though.
Being a great educator isn’t enough though. Hear what our families have to say about our amazing center!
Hear what our families have to say about our amazing center!
 – KinderCare Parent
– KinderCare Parent
 I can honestly say she is more than ready for Kindergarten. I’m so thankful that I found KinderCare Learning Center, Lake Arbor.
I can honestly say she is more than ready for Kindergarten. I’m so thankful that I found KinderCare Learning Center, Lake Arbor.
 Our centers aren’t just licensed—most are accredited, too! Find out more.
Our centers aren’t just licensed—most are accredited, too! Find out more. If your child has special dietary requirements and you would prefer to bring in their lunch, please make arrangements with the center director.
If your child has special dietary requirements and you would prefer to bring in their lunch, please make arrangements with the center director. That’s a big difference,
That’s a big difference, When your child is wandering all over the
When your child is wandering all over the Labels are everywhere to help kids connect
Labels are everywhere to help kids connect We welcome children ages 5–12 during school break times and make sure they have a
We welcome children ages 5–12 during school break times and make sure they have a Our original curriculum blends math,
Our original curriculum blends math, While your child experiments, they’ll discover how to use technology to do
While your child experiments, they’ll discover how to use technology to do
 He will be going to Kindergarten this upcoming school year and he is more then ready thanks to the teachers at KinderCare. He is very happy that he will be attending the after school program at KinderCare. I just want to thank the teachers at KinderCare for leading him in the right direction and for getting him ready for big boy school.
He will be going to Kindergarten this upcoming school year and he is more then ready thanks to the teachers at KinderCare. He is very happy that he will be attending the after school program at KinderCare. I just want to thank the teachers at KinderCare for leading him in the right direction and for getting him ready for big boy school. We are so proud to be their partner in parenting.
We are so proud to be their partner in parenting.
 Drop-in care may also be available. Reach out to your Center Director to learn more.
Drop-in care may also be available. Reach out to your Center Director to learn more.
 , 65
, 65  , 63
, 63  66 of the Tikhvin station of the Oktyabrskaya railway
66 of the Tikhvin station of the Oktyabrskaya railway Preschool daily
Preschool daily
 9mi
9mi
 7% YoY | May 2023
7% YoY | May 2023
 5 Baths | 1562 Sq. Ft.
5 Baths | 1562 Sq. Ft. Ft.
Ft.
 7% since last year. The median sale price per square foot in Kenmore is $88, up 4.1% since last year.
7% since last year. The median sale price per square foot in Kenmore is $88, up 4.1% since last year.
 S. bank. If you have an iOS device, and your card is registered to your Apple Wallet, Apple Pay will automatically display as a payment option within the McDonald’s app. If you have registered a card to the Google Pay™ app on your Android, you can select Google Pay™ as a payment method in the McDonald’s app. Payments with PayPal and Venmo are also available with Mobile Order & Pay.
S. bank. If you have an iOS device, and your card is registered to your Apple Wallet, Apple Pay will automatically display as a payment option within the McDonald’s app. If you have registered a card to the Google Pay™ app on your Android, you can select Google Pay™ as a payment method in the McDonald’s app. Payments with PayPal and Venmo are also available with Mobile Order & Pay. When you are checking out, choose the “Leave at Door” option in the Uber Eats app, “Leave at my door” option in the DoorDash app, or “contact-free delivery” in the Grubhub app, or choose the dropoff option “Leave order at my door” on Postmates.
When you are checking out, choose the “Leave at Door” option in the Uber Eats app, “Leave at my door” option in the DoorDash app, or “contact-free delivery” in the Grubhub app, or choose the dropoff option “Leave order at my door” on Postmates. Find more information in the recording notice FAQ.
Find more information in the recording notice FAQ.

 Ms. Schlange passed away on November 21, 2016.
Ms. Schlange passed away on November 21, 2016. Teaching teams also
Teaching teams also For more detailed information, please
For more detailed information, please

 Clair County preschool programs for children ages 0-5
Clair County preschool programs for children ages 0-5


 01.2022 N 18)
01.2022 N 18)  )
)  Yu., Kotukhov S.A.)
Yu., Kotukhov S.A.)  Petersburg
Petersburg
 Petersburg, Decree of the Government of St. Petersburg for 2023 from 29.11.2022 No. 1077
Petersburg, Decree of the Government of St. Petersburg for 2023 from 29.11.2022 No. 1077  Petersburg * (as amended on June 24, 2016) August 2016)
Petersburg * (as amended on June 24, 2016) August 2016) 

 ..1Disappointing
..1Disappointing Mrs. Kim or Mrs. Virginia greet you at the front desk with smiles on their faces. My favorite part about walking into Willow Bend is that sometimes Mr. Pilkington is there and he is always greeting me with a smile and stories about his journey through life. It encourages me to become a better person throughout all I do. The staff always encourages anyone they see to get through his or her schoolwork and do better in life.
Mrs. Kim or Mrs. Virginia greet you at the front desk with smiles on their faces. My favorite part about walking into Willow Bend is that sometimes Mr. Pilkington is there and he is always greeting me with a smile and stories about his journey through life. It encourages me to become a better person throughout all I do. The staff always encourages anyone they see to get through his or her schoolwork and do better in life.  I know that whenever they or I graduate, we will still be in touch and meeting up to hang out.
I know that whenever they or I graduate, we will still be in touch and meeting up to hang out. 
 To this day, he has not called her parents regarding her dismissal, and the only contact was a letter which came a week later. This type of behavior from a professional educator is unacceptable. Additionally, their tuition policy will not allow prorated refunds under any circumstances, so be prepared to throw away up to $7,000 for the semester if there are any issues
To this day, he has not called her parents regarding her dismissal, and the only contact was a letter which came a week later. This type of behavior from a professional educator is unacceptable. Additionally, their tuition policy will not allow prorated refunds under any circumstances, so be prepared to throw away up to $7,000 for the semester if there are any issues This is chosen according to the student’s ability.
This is chosen according to the student’s ability. The shorter days help me say pace through the day.
The shorter days help me say pace through the day. It turns out that I was wrong. I ended up loving their method of schooling. This school has helped me manage my time for both school and my personal life. I feel like I am a far more efficient person now. These time management skills will greatly help me for college and the rest of my life.
It turns out that I was wrong. I ended up loving their method of schooling. This school has helped me manage my time for both school and my personal life. I feel like I am a far more efficient person now. These time management skills will greatly help me for college and the rest of my life. I also thoroughly enjoy the devotionals that we have three times a week. This school is an overall great environment to learn about the Lord Jesus Christ. I strongly encourage you to enroll your child in Willow Bend Academy if you get the opportunity. I promise that you will not regret it.
I also thoroughly enjoy the devotionals that we have three times a week. This school is an overall great environment to learn about the Lord Jesus Christ. I strongly encourage you to enroll your child in Willow Bend Academy if you get the opportunity. I promise that you will not regret it.
 The atmosphere of this school is very familiar. This school has a morning class and an afternoon class, and students choose whichever they would like to join. The school time is about 4 hours, meaning the students can have a lot of free time for self-development. In my case, I’ve chosen the afternoon class, and I spend my morning time reading the Bible and practicing the guitar.
The atmosphere of this school is very familiar. This school has a morning class and an afternoon class, and students choose whichever they would like to join. The school time is about 4 hours, meaning the students can have a lot of free time for self-development. In my case, I’ve chosen the afternoon class, and I spend my morning time reading the Bible and practicing the guitar.
 I hope you readers consider this school when you choose the school you will go to. I especially recommend this school to those who need personal time and those who need special care from teachers.
I hope you readers consider this school when you choose the school you will go to. I especially recommend this school to those who need personal time and those who need special care from teachers. This small classroom setting allows the teachers to work more one-on-one with the students than in a traditional public school setting, letting the teachers teach towards each individual student in the way he/she can learn. The school accepts a student where he/she is and finds the best curriculum and educational plan that will suit his/her ability and needs. Students will be challenged in a way that will help them grow academically and achieve at their highest level possible. Additionally, the intimate setting between the teachers and students creates close relationships, allowing students to feel comfortable in seeking their teachers to help them with non-academic and more personal matters. The teachers use this opportunity, as well as through daily assemblies, to act as role models and mentors for the students and to help build strong character, work ethic, and morals. Students gain more than an education at Willow Bend Academy. The dedicated faculty, staff, and administration strive to prepare all students for the next stage in a student’s life, whether that be a different high school, college, a job, the military, or other diverse life path.
This small classroom setting allows the teachers to work more one-on-one with the students than in a traditional public school setting, letting the teachers teach towards each individual student in the way he/she can learn. The school accepts a student where he/she is and finds the best curriculum and educational plan that will suit his/her ability and needs. Students will be challenged in a way that will help them grow academically and achieve at their highest level possible. Additionally, the intimate setting between the teachers and students creates close relationships, allowing students to feel comfortable in seeking their teachers to help them with non-academic and more personal matters. The teachers use this opportunity, as well as through daily assemblies, to act as role models and mentors for the students and to help build strong character, work ethic, and morals. Students gain more than an education at Willow Bend Academy. The dedicated faculty, staff, and administration strive to prepare all students for the next stage in a student’s life, whether that be a different high school, college, a job, the military, or other diverse life path. They want all of their students to have a positive experience with Willow Bend Academy and to see their students succeed in their post high school life goals.
They want all of their students to have a positive experience with Willow Bend Academy and to see their students succeed in their post high school life goals. Willowbend provides an environment for ALL children to learn at their own pace in the best way for them to learn. Some students are able to move faster while others move a little bit slower. #2. The student ratio is 8 students per teacher. I love this because it allows students to have 1 on 1 tutoring and teaching time everyday if they need it and as they need it. Some students need this type of attention while others do not.. #3. I have observed many of our teachers who go over and beyond their written/formal responsibilities via tutoring during their lunch time and sometimes/many times after school. They really care and want to make sure that the student is learning the material, not just memorizing. #4. The teachers really, really care when the student is absent or even tardy. The front desk will make a call and the teacher will call many times also to check on a student. #5 EVERY student has the opportunity to really develop a rewarding relationship with their teacher.
Willowbend provides an environment for ALL children to learn at their own pace in the best way for them to learn. Some students are able to move faster while others move a little bit slower. #2. The student ratio is 8 students per teacher. I love this because it allows students to have 1 on 1 tutoring and teaching time everyday if they need it and as they need it. Some students need this type of attention while others do not.. #3. I have observed many of our teachers who go over and beyond their written/formal responsibilities via tutoring during their lunch time and sometimes/many times after school. They really care and want to make sure that the student is learning the material, not just memorizing. #4. The teachers really, really care when the student is absent or even tardy. The front desk will make a call and the teacher will call many times also to check on a student. #5 EVERY student has the opportunity to really develop a rewarding relationship with their teacher. #6 – EVERY student is IMPORTANT at Willowbend Academy. #7 Students have the opportunity at just about any time to walk in and talk to the principal. #8 The students learn how to set daily goals and plan out their week and month. This helps with college readiness. #9 Students are celebrated for mastering the material before moving on to the next book.
#6 – EVERY student is IMPORTANT at Willowbend Academy. #7 Students have the opportunity at just about any time to walk in and talk to the principal. #8 The students learn how to set daily goals and plan out their week and month. This helps with college readiness. #9 Students are celebrated for mastering the material before moving on to the next book. The teachers are terrific and the small learning environment is condusive to building supportive relationships with the faculty and students. We are very impressed with the curicullum and know our daughter is getting a great education. Willow Bend has been a trendous blessing to our family!!
The teachers are terrific and the small learning environment is condusive to building supportive relationships with the faculty and students. We are very impressed with the curicullum and know our daughter is getting a great education. Willow Bend has been a trendous blessing to our family!!
 com/Fotobank.com
com/Fotobank.com
 Happy for him.
Happy for him.  It’s like people don’t make mistakes.
It’s like people don’t make mistakes. 
 Very beautiful stamps!
Very beautiful stamps!  To tell the truth, what right do we have to go into the past and interfere in the affairs of people who lived a hundred years ago? Just imagine what it will be for them, for their psychology, for their whole life!
To tell the truth, what right do we have to go into the past and interfere in the affairs of people who lived a hundred years ago? Just imagine what it will be for them, for their psychology, for their whole life!  With these pills, she could live an extra ten or twenty years. And it doesn’t mean anything for our chaotic future, does it? What happens, I don’t know. Maybe it will save us. It may hasten our demise. Maybe it won’t have any effect. Understand yourself.
With these pills, she could live an extra ten or twenty years. And it doesn’t mean anything for our chaotic future, does it? What happens, I don’t know. Maybe it will save us. It may hasten our demise. Maybe it won’t have any effect. Understand yourself.  And the signature is Jackson. Is it Jackson Forbes? Maybe the name was passed down from generation to generation?
And the signature is Jackson. Is it Jackson Forbes? Maybe the name was passed down from generation to generation? 