Infant education: Infant Education Curriculum – Overview
Learning, Play, and Your Newborn (for Parents)
en español: Aprendizaje, juego y su recién nacido
Reviewed by: Mary L. Gavin, MD
Play is the main way that infants learn how to move, communicate, socialize, and understand their surroundings. During the first month of life, your baby will learn by interacting with you.
The first thing your baby will learn is to associate you with getting their needs met. So, the feel of your touch, the sound of your voice, and the sight of your face will begin to mean nourishment, warmth, and comfort.
Even at this young age, babies are ready to learn about the world around them. Your newborn loves to look your face. Newborns can recognize and respond to a parent’s voice (or other interesting sounds) by looking alert and becoming less active. Babies may try to find out where a sound is coming from by looking around.
When is My Baby Ready to Play and Learn?
During the first month of life, your newborn will spend much of the day sleeping or seeming drowsy. Over the next several weeks to months, your baby will begin to be awake and alert for longer periods of time. You’ll learn to recognize when your baby is ready to learn and play:
- A baby who is quiet and alert will be attentive and responsive and interested in their surroundings. Encourage learning with smiles, soothing sounds, and gentle caresses.
- A baby who is awake but active (squirming, flapping arms, or kicking legs) or fussing is less able to focus on you. The baby may seem upset or cry when you try to get their attention. These are signs that your baby may be getting hungry, tired, or overstimulated.
How Can I Help My Newborn Learn?
As you care for your newborn, talk, smile, and interact with your baby. Pay attention and respond to your baby’s cues. For example, watch how your baby moves or starts to make sounds back when you speak. Take turns “talking” to each other. This is how your baby learns to communicate.
In the first few weeks, you may want to introduce some simple, age-appropriate toys that appeal to the senses of sight, hearing, and touch, such as:
- rattles
- textured toys
- musical toys
- unbreakable crib mirrors
Choose toys and mobiles with contrasting colors and patterns.
How Can I Help My Newborn Play?
Here are some other ideas for encouraging your newborn to learn and play:
- Smile, stick out your tongue, and make other expressions for your infant to study, learn, and imitate.
- Use a favorite toy for your newborn to focus on and follow, or shake a rattle for your infant to find.
- Let your baby spend some awake time lying on the tummy to help strengthen the neck and shoulders. Always supervise your infant during “tummy time” and be ready to help if they get tired or frustrated in this position. Never put an infant to sleep on their stomach — babies should sleep on their backs to reduce the risk of SIDS (sudden infant death syndrome).
- Talk and read to your baby.
- Put on soothing music and hold your baby, gently swaying to the tune.
- Pick a soothing song or lullaby and softly sing it often to your baby. The familiarity of the sound and words will have a soothing effect, particularly during fussy times.
When Should I Call the Doctor?
There is a wide range of normal development, so some children may gain skills earlier or later than others. Talk to your doctor if you have any concerns about how your newborn sees and hears, or if you have any questions or concerns about your baby’s development.
Reviewed by: Mary L. Gavin, MD
Date reviewed: May 2022
Share:
/content/kidshealth/misc/medicalcodes/parents/articles/learnnewborn
Resources for Infant Educarers®Resources for Infant Educarers® (RIE®)
Parent-Infant Guidance: RIE Certified Parent-Infant Guidance classes are designed to provide an environment where babies can be attentive, active, exploring and aware of self and others.
Pasadena Schedule
Monday
Instructor: Kira Solomatova
– 12:30 Young toddler (pre-walking/walking)
Tuesday
Instructor: Kira Solomatova
– 9:30 Toddler (pre-walking/newly walking/walking)
Wednesday
Instructor: Ruth Anne Hammond
– 9:30 Young Toddler (pre-walking/newly walking/walking)
Thursday
Instructor: Ruth Anne Hammond
– 9:30 Toddler (newly walking/walking)
– 1:30 Young Infant (pre or newly mobile) *new class forming!
Saturday
Instructor: Kira Solomatova
– 9:30 Toddler (newly walking/walking) *WAITLIST ONLY
– 12:30 Older infant (mobile)*ONE spot left!
Sunday
Instructor: Jill Getto Lee
– 9:30 Older Toddler (walking)
– 12:30 Young Toddler (newly walking/walking)
Hollywood Schedule
Tuesday
Instructor: Wendy Kronick
– 11:00 Young toddler (mobile/newly walking)
Wednesday
Instructor: Wendy Kronick
– 9:30 Older Toddler (walking)
Thursday
Instructor: Jill Getto Lee
– 12:30 infant (mobile) *new class forming
Saturday
Instructor: Ida Reid
– 10:00 Toddler (newly walking/walking)
-12:30 Young Infant (pre-mobile/mobile) *new class forming
– 3:00 Older Toddler (walking) *WAITLIST ONLY
Sunday
– 12:00 Young infant (pre-mobile/newly mobile)* ONE spot left!
Our online classes are facilitated by a certified RIE Associates where small groups of no more than 8 families of similarly-aged children come together to discuss relevant developmental topics.
- Online class information
- Access our free orientation videos
- Check out our FAQs
- Send questions to [email protected]
- Register now
Monday
12:30 PM Parents of older toddlers/young preschoolers (28 – 47 months)
Wednesday
6:00 PM Parents of young toddlers (14 to 15 months)
Thursday
10:30 AM Parents of older infants (9 to 10 months)
7:00 PM Parents of young preschoolers (20 to 28 months)
Friday
9:30 AM Parents of toddlers (13 to 22 months)
Saturday
10:00 AM Young infants (newborn to 7 months)
11:30 AM Parents of preschoolers (23 to 30 months) *WAITLIST ONLY
Sunday
11:30 AM Parents of preschoolers (29 to 39 months)
**All times listed are in the Pacific time zone.
We have several class options for parents and professionals that support our mission: To improve the lives of infants and toddlers through respectful care.
Introduction to Educaring: This 3-hour course offers an overview of Educaring, instructed by a certified RIE® Associate. Topics include trust in the child, the guidelines of sensitive caregiving, facilitating optimal development through play, and communicating respect for children through our everyday interactions.
Before Baby: An introductory online course for those expecting, waiting to adopt, or thinking about becoming a parent, Before Baby™ is designed to start you on your journey with confidence in yourself as a parent and trust in your baby’s unique ability to show you the way.
Nurturing Nanny: This course is for in-home caregivers and offers knowledge and practical suggestions that can help make this work easier and more enjoyable, resulting in advantages for the infants and young children who receive professional care.
RIE Foundations: Theory and Observation: This professional development course is offered online, at our Los Angeles based RIE Center and throughout the world. It is designed to enhance the skills and competencies of parents, and professionals who work in the field of infant care, teach in a college environment, work with parents, or train students in infant care and development.
Join our Mailing list
Magda Gerber founded RIE® in 1978
“The infant Magda showed us is so much more; she showed us that a baby is a miracle, a whole person, who, with our deeply attentive care, unfolds into a wonder, unique in the world. She taught us to wait, to watch without preconception, to observe with genuine curiosity, to see what the baby was trying to tell us. She gave us new eyes through which to see, not the infant we have in mind, but the actual infant before us, and to respond quietly, gently, slowly to its cues and initiations, and to respond not only to its needs but its competencies as well.
Read more
“Observe more, do less, enjoy most.” -Magda Gerber
Infantile hemangioma: methods of treatment of infantile hemangioma
Infantile hemangioma, also called infantile, is a fairly common skin pathology that occurs in children. This is a benign formation that is present in newborns or may appear in an infant in the first months of life. In most cases, this vascular formation does not require treatment. But sometimes the need to remove the pathology is due to its large size or anatomical location. For example, an extensive infantile hemangioma on the face can lead to problems with vision, muscle development. And it can also cause increased attention of others to the child, which will subsequently develop into complexes.
Medical statistics: Infantile hemangioma occurs in 5% of term infants and 20% of preterm infants. This type of vascular pathology is more common in girls than in boys.
Causes of infantile hemangioma
Causes of formation such as infantile hemangioma are due to oxygen deficiency, its non-receipt in the required volumes by blood vessels. Scientists among the causes of the development of pathology call placental insufficiency, multiple pregnancy, infectious diseases, unstable hormonal levels and anemia in the mother during childbearing.
Clinical picture
Most often, infantile hemangioma appears in the first days after birth. The first symptom is the expansion of the vessels of the skin in a small area of the body. It manifests itself as a bright spot with protruding capillaries in the middle. The first stage of education development can take several months. At this time, it grows. After 3-4 months, the neoplasm becomes bright red. When the baby is stressed, for example, screaming, taking a hot bath, the spot looks swollen. At the next stage, the growth of education slows down. At the age of 12 months, the spot stops growing.
Spot brightens, decreases in size. In nine out of ten cases, self-healing occurs. By the age of 9, the formation may completely disappear. More precisely, the neoplasm acquires skin color. In some cases, a bright spot, a scar, remains at the site of the pathology.
Classification of formations of this species
Formations of this species may be single or multiple. Neoplasms are localized on any parts of the skin and mucous membranes. Doctors divide children’s hemangiomas into the following types:
- Local form accounts for 90% of all cases. Education has clear boundaries. Hemangioma grows from one point. Local neoplasms are superficial, not germinating in tissues, deep subcutaneous and combined, growing on the surface of the skin and in its depths.
- The segmental form of pathology is characterized by an extensive size. Such formations appear much less often than local ones. They are not visible at birth, but appear quickly in the first weeks of life.
When a segmental form is detected, a thorough examination of the child is recommended, since pathology is often evidence of serious health problems.
- A special form of formation is called “congenital”, since the baby is born with an already fully formed formation. A feature of the disease is complete self-healing by the third year of life.
- Congenital non-vanishing hemangioma is present in the baby at the time of birth, but does not disappear over the years. Its feature is a constant size. The growth does not grow or decrease over time.
As a rule, education does not bother babies. However, in some cases, the physiological location of the hemangioma requires mandatory treatment. For example, if the pathology is located in the eye area, it can reduce vision, if it appears on the face, difficulties may arise with the correct functioning of facial muscles. Hemangioma on the ear leads to deformation of the shell, its increase. Deep hemangioma of the external genitalia leads to ulceration of the skin.
Diagnosis of infantile hemangioma
The diagnosis is established after clinical examination. When diagnosing pathology, the doctor must identify the hemangioma, excluding other tumor and vascular diseases (fiery nevus, pyogenic granuloma, vascular malformations and other neoplasms). The doctor also determines the stage of the disease. Angiography, evaluation of blood flow, and a blood coagulation test may be required to clarify the child’s condition. As a rule, histology is not performed for this anomaly.
Treatment of infantile hemangioma
The decision to treat infantile hemangioma is made by the parents after consultation with a dermatologist. If the formation grows in an uncomplicated area of the body, does not impede vital functionality, there is no need for treatment. Dynamic observation will be sufficient in order not to miss dangerous complications. Expectant tactics provides for regular monitoring by a doctor with fixing changes.
Important: Parents often worry that education is growing, and the pediatrician or dermatologist is not treating her. With children’s hemangiomas, this tactic is justified, since there is a high probability of self-healing with minimal aesthetic complications.
With the growth of a neoplasm in difficult areas (the area of the eyes, lips, nose, genitals), it is necessary to remove the formation. This measure helps to prevent health problems in the future.
Effective methods of anomaly removal are laser therapy, cryotherapy (liquid nitrogen freezing), surgery. The use of liquid nitrogen and surgery are inferior to laser therapy, as only it gives a highly effective result without side effects and complications. An experienced doctor can easily control the intensity and depth of the beam exposure. After the operation, there are no scars and scars. The procedure is performed without general anesthesia. It is also important that laser treatment eliminates the risk of bleeding, infection.
Important: Laser treatment of infantile hemangiomas has a good prognosis. Education disappears without a trace. To see this, just look at the photo of the skin of our little patients before and after the operation.
Treatment of infantile hemangiomas in Kharkiv
Mole Diagnostic Center “Lazersvit” offers diagnostics, observation and removal of infantile hemangiomas by laser method. We invite you to sign up for a consultation with a dermatologist if you have found this pathology in your child. The doctor will conduct an examination, determine the type of disease, and evaluate whether it is necessary to treat the formation in a particular small patient.
Important: Urgent surgery is required if hemangioma is bleeding. A vascular formation may begin to bleed spontaneously or with trauma.
Our clinic in Kharkov is the best specialized center, the advantages of which are qualified personnel. We use a modern laser for the treatment of various skin pathologies and demonstrate reasonable prices for all procedures.
Infantile hemangioma — SPb GBUZ KDCD
Infantile (infantile) hemangioma is a benign vascular tumor that can be congenital in a child, or grow in the first weeks of his life. (International Society for the Study of Vascular Anomalies)
Infantile hemangiomas occur in about 3% to 5% of full-term newborns and in about 22% of preterm infants whose birth weight was less than 1 kg. Girls are affected about three times more often than boys. Infantile hemangiomas that grow in only one limited area (local hemangioma)
are much more common – 90% of cases than extensive hemangiomas (segmental hemangiomas) – 10% involution (stop growth, or stabilization ),

Classification:
Type:
- Surface
- Deep Mixed
(surface + deep) - Reticular (abortive)
- with minimal growth, etc.
Shape:
- Focal
- Multiple
- Segmental
- Borderline
Special forms:
- congenital rapidly self-limiting hemangioma;
- congenital non-involving;
- benign neonatal hemangiomatosis;
Treatment:
Options
- drug treatment with beta-blockers (drug propranalol)
- laser therapy
- cryotherapy
- surgery
If the hemangioma grows in a simple anatomical area of the body and it does not limit vital functions (for example, hemangiomas on the arms, legs, trunk), then there is no need for treatment.
If they grow rapidly in complex critical areas, then they must be treated to avoid complications. For example, infantile hemangioma of the eye area (threat of reduction / loss of vision), lips area (does not completely disappear or disappear slowly) and nose area (in children increased risk of nasal deformity).
- avoid complications associated with a serious cosmetic defect or limitation of vital functions
- treat necrosis (hemangiomas ulceration),
- slow down/stop the growth of hemangiomas,
- accelerate the recovery process of large infantile hemangiomas.
The examination and management protocol consists of 4 steps.
At stage I, indications for systemic treatment of infantile hemangiomas with propranolol are identified, a basic examination is performed, including an examination of the cardiovascular system, and, in the absence of contraindications, propranolol therapy is prescribed with a gradual dose titration of the drug. In parallel, the presence or absence of undesirable effects during therapy is monitored. One of the most important studies at this stage is ultrasound (the thickness of the vascular formation and the number of vessels are determined; in the Doppler mode, the linear blood flow velocity (LBV) and the resistance index in the feeding and intraparenchymal vessels are evaluated.
Stage II treatment is carried out on an outpatient basis under the supervision of a pediatrician and a pediatric cardiologist. It consists in taking the drug correctly and regularly, adjusting its dose against the background of a changing body weight of the child, conducting regular examinations and photographic documentation.
Stage III – dynamic inpatient examination, which is carried out every 3 months during the entire period of treatment, as well as after its completion. Stage III includes a cardiological and general clinical examination, as well as dynamic ultrasound of the vessels. In addition, the dose of the drug is adjusted, possible undesirable cardiac and extracardiac effects are recorded, and a decision is made on the timing of completion of therapy.
Stage IV begins after discontinuation of propranolol therapy, when the child is again examined. At this stage, it is important to exclude the presence of withdrawal syndrome (relapses).
Laser therapy
Impulse laser on dyes with a ramp lamp (FDPL system)
and IPL pulsed lamp is recommended when infant hemangiymmas, small size and they grow on a limited body of cryotherapy
,
in Germany, cryotherapy is a standard method
treatment for small, flat infantile hemangiomas with a maximum diameter of
1 cm.








 When a segmental form is detected, a thorough examination of the child is recommended, since pathology is often evidence of serious health problems.
When a segmental form is detected, a thorough examination of the child is recommended, since pathology is often evidence of serious health problems. 
 2) has been employed as an assistant child care teacher since 2/22/18.
2) has been employed as an assistant child care teacher since 2/22/18. 06(2)(b)
06(2)(b) 07(3)(a)4.
07(3)(a)4. 09(4)(b)
09(4)(b) In addition, an uncovered bucket of kitchen grease is observed on the floor in the center’s kitchen.
In addition, an uncovered bucket of kitchen grease is observed on the floor in the center’s kitchen.


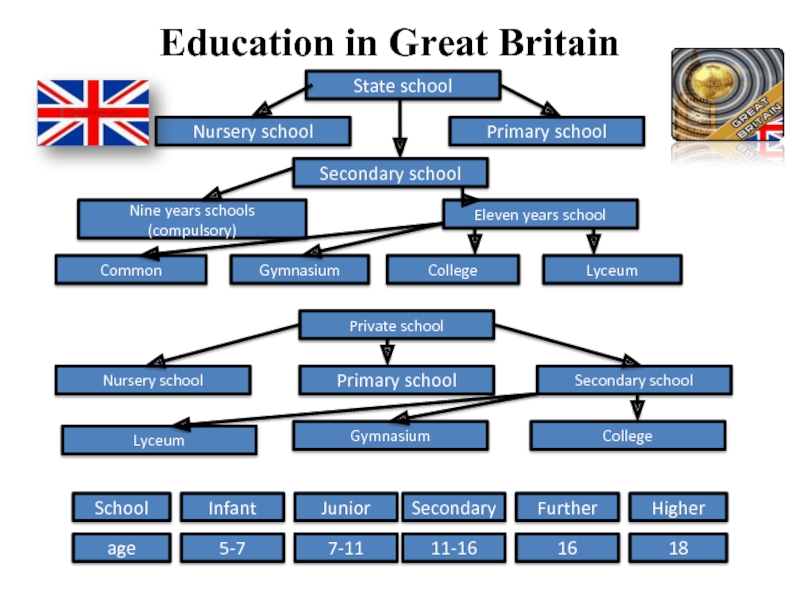
 There are two main solutions here. Stay in school and finish 10th and 11th grade or go to college and get a vocational education. I see certain advantages of the second option, namely:
There are two main solutions here. Stay in school and finish 10th and 11th grade or go to college and get a vocational education. I see certain advantages of the second option, namely: 
 The opening hours of the admissions office: Monday to Friday from 9:00 to 18:00.
The opening hours of the admissions office: Monday to Friday from 9:00 to 18:00.  02.02 Teaching in elementary grades
02.02 Teaching in elementary grades 
 More than 70 students showed their knowledge of the Italian language and successfully completed all the tests. SSBA students are the only ones in Togliatti who took part in the Universiade 2023 and showed no less excellent results!
More than 70 students showed their knowledge of the Italian language and successfully completed all the tests. SSBA students are the only ones in Togliatti who took part in the Universiade 2023 and showed no less excellent results!  The event was held by the SSBA psychologist Lyubov Vladimirovna Chernyaeva (clinical psychologist, art therapist, member of the Togliatti Association of Psychotherapists and Psychologists).
The event was held by the SSBA psychologist Lyubov Vladimirovna Chernyaeva (clinical psychologist, art therapist, member of the Togliatti Association of Psychotherapists and Psychologists).  Classes are held in various disciplines, incl. in an interactive way.
Classes are held in various disciplines, incl. in an interactive way.  861-18 dated May 4, 2018 series 63A 01 No. 0000917
861-18 dated May 4, 2018 series 63A 01 No. 0000917  The survey is conducted anonymously among managers, teachers and students of SVE educational programs.
The survey is conducted anonymously among managers, teachers and students of SVE educational programs.  The disclosure of these stories helps to understand more deeply how the British nation and the British Empire were formed, as well as the significance of the intellectual colonization of the Highlands for empire building overseas and, more broadly, the role of humanitarian knowledge in the age of Reason, Enlightenment and the first global empires. S.G. Malkin – Doctor of Historical Sciences, Professor of the Department of World History and Teaching Methods of the Volga Region State Social and Humanitarian Academy (Samara), author of more than 70 scientific works on history.
The disclosure of these stories helps to understand more deeply how the British nation and the British Empire were formed, as well as the significance of the intellectual colonization of the Highlands for empire building overseas and, more broadly, the role of humanitarian knowledge in the age of Reason, Enlightenment and the first global empires. S.G. Malkin – Doctor of Historical Sciences, Professor of the Department of World History and Teaching Methods of the Volga Region State Social and Humanitarian Academy (Samara), author of more than 70 scientific works on history. 
 .. The list is endless. And no matter what series you take, each of them is a finely built balance between relevance and research continuity, between courage and reverence for the science of the past, on the basis of which new concepts are formed.
.. The list is endless. And no matter what series you take, each of them is a finely built balance between relevance and research continuity, between courage and reverence for the science of the past, on the basis of which new concepts are formed.

 S. Since 1969, it has successfully served children with time-tested techniques and proven results.
S. Since 1969, it has successfully served children with time-tested techniques and proven results. We’re here to help our employees navigate the integration of work and life:
We’re here to help our employees navigate the integration of work and life:
 Fresh vacancies for today
Fresh vacancies for today
 00 to 19.00 from Monday to Friday; can also be retired; object Children’s … garden at Samara, Balkhash proezd 36 (Industrial district …
00 to 19.00 from Monday to Friday; can also be retired; object Children’s … garden at Samara, Balkhash proezd 36 (Industrial district …  ru
ru  Medical education. …
Medical education. …  … Education and upbringing of preschool children; observance of the daily routine and schedule at kindergarten kindergarten ; conducting developing … classes in accordance with the program for children kindergarten . …
… Education and upbringing of preschool children; observance of the daily routine and schedule at kindergarten kindergarten ; conducting developing … classes in accordance with the program for children kindergarten . …  ..
.. 
 Use filters to quickly
Use filters to quickly
 Group up to 10 children. Working hours from 7:00 to 19:00 from …
Group up to 10 children. Working hours from 7:00 to 19:00 from …  Shift work.
Shift work. 
 ..0013
..0013  Nanny required. Honey. book is required. For part-time work…
Nanny required. Honey. book is required. For part-time work… 
 82 miles
82 miles

 In addition to our authentic Montessori program, we offer Spanish immersion for all ages
In addition to our authentic Montessori program, we offer Spanish immersion for all ages
 For Toddler, Preschool, and Pre-kindergarten, Harper offers parents the flexibility to choose between programs that are full day or half-day. Parents can also choose how many days per week from two days up to five days. Morning and afternoon extended care is also available.
For Toddler, Preschool, and Pre-kindergarten, Harper offers parents the flexibility to choose between programs that are full day or half-day. Parents can also choose how many days per week from two days up to five days. Morning and afternoon extended care is also available.
 cdss.ca.gov/inforesources/Child-Care-Licensing
cdss.ca.gov/inforesources/Child-Care-Licensing services
services  In addition, even babies are accepted here.
In addition, even babies are accepted here.
 club
club
 ..
.. 

 Content delivery is primarily asynchronous in nature and entirely online. At the middle school level, daily synchronous morning meetings with GVA staff will be held Monday-Thursday. These meetings are optional. Teachers and a GVA Academic Coach will be available for office hours for students to offer support. Students can expect to be in online classes with other students from across the state of Kansas. Blue Valley students will not all be in the same class(es.)
Content delivery is primarily asynchronous in nature and entirely online. At the middle school level, daily synchronous morning meetings with GVA staff will be held Monday-Thursday. These meetings are optional. Teachers and a GVA Academic Coach will be available for office hours for students to offer support. Students can expect to be in online classes with other students from across the state of Kansas. Blue Valley students will not all be in the same class(es.)  Elementary students will take art first semester and physical education the second semester.
Elementary students will take art first semester and physical education the second semester.

 While the case manager will not change, the accommodations and modifications to the general education materials will be made by a special education teacher and/or paraprofessional contracted by Blue Valley but not assigned to the home school.
While the case manager will not change, the accommodations and modifications to the general education materials will be made by a special education teacher and/or paraprofessional contracted by Blue Valley but not assigned to the home school. (In rare instances, the school can work with district leaders to allow proof in the form of other legal documents, such as a Green Card, for up to 30 days until a certified copy of the birth certificate must be provided.)
(In rare instances, the school can work with district leaders to allow proof in the form of other legal documents, such as a Green Card, for up to 30 days until a certified copy of the birth certificate must be provided.)


 Please note there will be a $250 maximum payable amount for families with multiple Blue Valley students. This fee helps support all sports, activities, clubs and other supplemental contract items that require extra-duty supervision from qualified district staff. It only covers a portion of the costs for a student team activity and does not replace fees currently being charged for programs such as drill team, cheerleading, certain clubs or sports.
Please note there will be a $250 maximum payable amount for families with multiple Blue Valley students. This fee helps support all sports, activities, clubs and other supplemental contract items that require extra-duty supervision from qualified district staff. It only covers a portion of the costs for a student team activity and does not replace fees currently being charged for programs such as drill team, cheerleading, certain clubs or sports. Fee amounts will be finalized and assigned when official schedules are available in August.
Fee amounts will be finalized and assigned when official schedules are available in August. KAZINFORM – The concept of storage and circulation of cryptocurrencies was developed in Kazakhstan. This was announced by Asylbek Davletov, Director of the FinTech Regulation Department of the Astana International Financial Center, Kazinform correspondent reports.
KAZINFORM – The concept of storage and circulation of cryptocurrencies was developed in Kazakhstan. This was announced by Asylbek Davletov, Director of the FinTech Regulation Department of the Astana International Financial Center, Kazinform correspondent reports.  According to him, many jurisdictions are currently considering the possibility of adopting appropriate amendments or even separate laws to regulate this type of fundraising.
According to him, many jurisdictions are currently considering the possibility of adopting appropriate amendments or even separate laws to regulate this type of fundraising.  Today we already have concrete implemented projects,” he said.
Today we already have concrete implemented projects,” he said.  ..
..  ..
.. 
 Tired Tortilla was dragged…Collapse)
Tired Tortilla was dragged…Collapse)  station. We sit in a modern trolleybus with huge windows and go to Kaspiysk, which stretches along the sea. ( Passing through the wide … Collapse )
station. We sit in a modern trolleybus with huge windows and go to Kaspiysk, which stretches along the sea. ( Passing through the wide … Collapse )  In the morning Tortilla, having had a rest, was so excited that she agreed to go to the Kargashil Sever pass, thus replacing the Khunguf pass, but on one condition that we would not directly cross the stone dunes of the plateau (the stone “fur coat” of the retreating Bulunga l.).
In the morning Tortilla, having had a rest, was so excited that she agreed to go to the Kargashil Sever pass, thus replacing the Khunguf pass, but on one condition that we would not directly cross the stone dunes of the plateau (the stone “fur coat” of the retreating Bulunga l.).  Having returned on September 1 from the first trip, having washed up and having a bit of a meal, we thought about the next trip. Why not wait until next summer? Yes, and the awl in one place began to tingle intensely, calling us on the road. We quickly zabatsal as always a short route, threw backpacks into the car of our good friend, a horse rider, and … forward to the mountains.
Having returned on September 1 from the first trip, having washed up and having a bit of a meal, we thought about the next trip. Why not wait until next summer? Yes, and the awl in one place began to tingle intensely, calling us on the road. We quickly zabatsal as always a short route, threw backpacks into the car of our good friend, a horse rider, and … forward to the mountains. 
 After giving birth, queens can get pregnant after two weeks.
After giving birth, queens can get pregnant after two weeks. She is a professional member of the Cat Writers’ Association, won the prestigious PurinaOne Health Award for her writing. Franny has also authored two books on cat care.
She is a professional member of the Cat Writers’ Association, won the prestigious PurinaOne Health Award for her writing. Franny has also authored two books on cat care.
 This usually occurs at around three weeks into the pregnancy. There may be a slight discharge from the nipples, as well.
This usually occurs at around three weeks into the pregnancy. There may be a slight discharge from the nipples, as well. It can be a little harder to spot an enlarging belly if your cat was overweight to begin with, however.
It can be a little harder to spot an enlarging belly if your cat was overweight to begin with, however. Line the box with a few soft blankets that can be disposed of or washed as they become soiled.
Line the box with a few soft blankets that can be disposed of or washed as they become soiled. This is a minor amount of radiation that will not be harmful to the kittens or the mother. Kitten spines and skulls begin to be visible on x-rays after about 42 days into the pregnancy.
This is a minor amount of radiation that will not be harmful to the kittens or the mother. Kitten spines and skulls begin to be visible on x-rays after about 42 days into the pregnancy. Watch from a safe distance to make sure she does not go into distress. Generally, the first stage of a cat’s labor lasts an average of six to 12 hours, and is the period in which contractions begin and the cervix opens. The second stage of labor is the actual delivery of the kittens. There can be anywhere from 10 minutes to an hour between each kitten’s birth. After the delivery of each kitten, the queen will experience the third stage of labor, which includes the delivery of the placenta. It can take anywhere from two hours to more than a day for a cat to finish giving birth once stage two begins, but two to six hours is common.
Watch from a safe distance to make sure she does not go into distress. Generally, the first stage of a cat’s labor lasts an average of six to 12 hours, and is the period in which contractions begin and the cervix opens. The second stage of labor is the actual delivery of the kittens. There can be anywhere from 10 minutes to an hour between each kitten’s birth. After the delivery of each kitten, the queen will experience the third stage of labor, which includes the delivery of the placenta. It can take anywhere from two hours to more than a day for a cat to finish giving birth once stage two begins, but two to six hours is common.
 She may go in and out of her nesting area, almost as if pacing.
She may go in and out of her nesting area, almost as if pacing. The average feline litter is four to six kittens, and the mother will clean each newborn thoroughly as it emerges. The kittens should begin to nurse within an hour of birth. If your cat appears to be very distressed, straining, or unable to care for her kittens, contact your veterinarian for advice.
The average feline litter is four to six kittens, and the mother will clean each newborn thoroughly as it emerges. The kittens should begin to nurse within an hour of birth. If your cat appears to be very distressed, straining, or unable to care for her kittens, contact your veterinarian for advice.
 Veterinary Clinics Of North America: Small Animal Practice, vol 42, no. 3, 2012, pp. 445-456. Elsevier BV, doi:10.1016/j.cvsm.2012.01.010
Veterinary Clinics Of North America: Small Animal Practice, vol 42, no. 3, 2012, pp. 445-456. Elsevier BV, doi:10.1016/j.cvsm.2012.01.010 However, be careful: this phenomenon is also observed in false pregnancy.
However, be careful: this phenomenon is also observed in false pregnancy.  Fetal movement can often be seen or felt by hand through the abdominal wall.
Fetal movement can often be seen or felt by hand through the abdominal wall.  nine0003
nine0003  nine0003
nine0003 
 nine0003
nine0003  Domestic cats are able to bear offspring up to three times a year, but this, of course, is a great stress for their body. According to veterinarians, it is advisable for a cat to bring kittens into the world no more than once a year. nine0003
Domestic cats are able to bear offspring up to three times a year, but this, of course, is a great stress for their body. According to veterinarians, it is advisable for a cat to bring kittens into the world no more than once a year. nine0003  nine0003
nine0003  Putting your hand on her stomach, you can feel the kittens moving. By the end of the term, the stomach drops: it used to start right behind the ribs, and now it is located in the hips. The cat constantly follows the owner and at the same time begins to look for a place for a nest. By the way, it is worth taking care of it in advance. nine0003
Putting your hand on her stomach, you can feel the kittens moving. By the end of the term, the stomach drops: it used to start right behind the ribs, and now it is located in the hips. The cat constantly follows the owner and at the same time begins to look for a place for a nest. By the way, it is worth taking care of it in advance. nine0003  nine0003
nine0003 
 59 miles
59 miles
 11 miles
11 miles
 24 miles
24 miles
 66 miles
66 miles
 80 miles
80 miles
 22 miles
22 miles
 11 miles
11 miles
 20 miles
20 miles
 44 miles
44 miles
 32 billion of Russian assets
32 billion of Russian assets  ” Blogger Liza Vasilenko returned to Russia
” Blogger Liza Vasilenko returned to Russia 
 The first batch of ungulates arrived in 2014 in the Podgorensky district. Valuable lean deer meat is not inferior in quality to pork and beef. Today, reindeer husbandry is considered as an alternative type of animal husbandry, which is associated with repeated outbreaks of African swine fever in the Voronezh region in 2013.
The first batch of ungulates arrived in 2014 in the Podgorensky district. Valuable lean deer meat is not inferior in quality to pork and beef. Today, reindeer husbandry is considered as an alternative type of animal husbandry, which is associated with repeated outbreaks of African swine fever in the Voronezh region in 2013.

 After the animals went through full customs clearance in Moscow, they were delivered to the farm in the village of Duginka, Bobrovsky District.
After the animals went through full customs clearance in Moscow, they were delivered to the farm in the village of Duginka, Bobrovsky District. 

 Ru
Ru

 ..
.. We believe it is our responsibility to help working parents raise their children to be well adjusted and happy Christian youth and adults by providing the best qual …
We believe it is our responsibility to help working parents raise their children to be well adjusted and happy Christian youth and adults by providing the best qual … This child care center helps with children in the age range of 6 WKS Through 14 YRS. The provider does not participate in a subsidized child care program.
This child care center helps with children in the age range of 6 WKS Through 14 YRS. The provider does not participate in a subsidized child care program. The provider does not participate in a subsidized child care program.
The provider does not participate in a subsidized child care program.
 This child care center helps with children in the age range of 6 WKS Through 6 YRS. The provider does not participate in a subsidized child care program.
This child care center helps with children in the age range of 6 WKS Through 6 YRS. The provider does not participate in a subsidized child care program.


 The object is to tilt the box so that the pom pom rolls through the tubes in number order.
The object is to tilt the box so that the pom pom rolls through the tubes in number order. Spin the wheel to show how the “-un” word ending can turn from “run” into “fun” or “bun.”
Spin the wheel to show how the “-un” word ending can turn from “run” into “fun” or “bun.”
 It’s a learning activity and wall art in one.
It’s a learning activity and wall art in one. The great thing about this game is that it’s so easy to pack up, it’s the perfect activity to bring to Grandma’s house.
The great thing about this game is that it’s so easy to pack up, it’s the perfect activity to bring to Grandma’s house. 
 Your toddler may become a picky eater, and you may worry that he or she is not eating enough. Remember, this is a normal, healthy response to your child’s decreased energy needs.
Your toddler may become a picky eater, and you may worry that he or she is not eating enough. Remember, this is a normal, healthy response to your child’s decreased energy needs. This helps provide good nutrition.
This helps provide good nutrition. Large amounts of food on the plate may discourage your toddler from trying new foods.
Large amounts of food on the plate may discourage your toddler from trying new foods. Please talk to your child’s doctor if you choose to feed your toddler a vegan diet. Dairy products and eggs can help provide needed protein and calcium.
Please talk to your child’s doctor if you choose to feed your toddler a vegan diet. Dairy products and eggs can help provide needed protein and calcium. Calcium-fortified orange juice, broccoli, sardines and tofu also contain calcium. Your child needs about 500 mg of calcium a day.
Calcium-fortified orange juice, broccoli, sardines and tofu also contain calcium. Your child needs about 500 mg of calcium a day. Please talk with your child’s pediatrician about choosing a supplement for your child.
Please talk with your child’s pediatrician about choosing a supplement for your child.
 There are steps parents can take to prevent mealtime battles over picky eating habits. Read on.
There are steps parents can take to prevent mealtime battles over picky eating habits. Read on.
 Learn about other milestones.
Learn about other milestones.
 The child changes along with the surrounding reality and the pedagogical methods of involving him in learning that have been tested for many decades cease to act on him, and the school has not proposed a new approach to organizing the involvement of the child in the educational process. nine0003
The child changes along with the surrounding reality and the pedagogical methods of involving him in learning that have been tested for many decades cease to act on him, and the school has not proposed a new approach to organizing the involvement of the child in the educational process. nine0003  nine6% of respondents in large cities, in medium and small – 93%, and in villages – up to 85%.
nine6% of respondents in large cities, in medium and small – 93%, and in villages – up to 85%.  They are located in specialized premises, classes are conducted by specialists with specialized thematic education and additional pedagogical training, modern teaching methods and technical base are used. This model underlies the activities of our Academy.
They are located in specialized premises, classes are conducted by specialists with specialized thematic education and additional pedagogical training, modern teaching methods and technical base are used. This model underlies the activities of our Academy. 
 Extra classes should not adversely affect school performance. Parents should decide and choose a priority direction for organizing leisure activities, abandon some of the secondary activities that may need to be transferred to another period of the child’s development; nine0046
Extra classes should not adversely affect school performance. Parents should decide and choose a priority direction for organizing leisure activities, abandon some of the secondary activities that may need to be transferred to another period of the child’s development; nine0046
 nine0046
nine0046

 Also, these classes can be a great help in the additional education of children attending regular kindergartens, where the main goal is to look after children, and not their development. nine0003
Also, these classes can be a great help in the additional education of children attending regular kindergartens, where the main goal is to look after children, and not their development. nine0003  They are easily carried away by new ideas and activities. This is just the best time to see your child’s preferences, as well as to give the baby to go in different directions, to feel different. nine0003
They are easily carried away by new ideas and activities. This is just the best time to see your child’s preferences, as well as to give the baby to go in different directions, to feel different. nine0003  In this case, for many children, language learning is one of the most difficult subjects. In this case, the benefits of an additional game lesson in learning foreign languages become obvious. Playing with languages, one might say, from the cradle, your baby will be happy to attend classes at school in later years. nine0003
In this case, for many children, language learning is one of the most difficult subjects. In this case, the benefits of an additional game lesson in learning foreign languages become obvious. Playing with languages, one might say, from the cradle, your baby will be happy to attend classes at school in later years. nine0003  nine0003
nine0003 
 Stop the spending cycle with this easy DIY cat-wand tutorial.
Stop the spending cycle with this easy DIY cat-wand tutorial. It can be a small enclosure that juts out of an apartment or a larger structure built from the ground up.
It can be a small enclosure that juts out of an apartment or a larger structure built from the ground up.
 And if your cat isn’t a fan, they’re beautiful enough to use as décor! Make your own.
And if your cat isn’t a fan, they’re beautiful enough to use as décor! Make your own.
 And in it we will tell you how to take your restless mustachioed. It is unlikely that he will resist all sorts of funny bright things that are not difficult to make with your own hands. Let’s get started!
And in it we will tell you how to take your restless mustachioed. It is unlikely that he will resist all sorts of funny bright things that are not difficult to make with your own hands. Let’s get started! 
 Balls, beads, hanks, spools of thread are a great option.
Balls, beads, hanks, spools of thread are a great option.  Now cat trinkets have their place of honor: like live rattles, they playfully hang on the rack, entertaining the indefatigable animal.
Now cat trinkets have their place of honor: like live rattles, they playfully hang on the rack, entertaining the indefatigable animal. 

 It is only necessary to connect them with the help of corner elements, which are sold in any hardware store. You will also need to cut holes in the pipes a little more than the paws of cats, and put various little things inside. The cat will try to get them.
It is only necessary to connect them with the help of corner elements, which are sold in any hardware store. You will also need to cut holes in the pipes a little more than the paws of cats, and put various little things inside. The cat will try to get them. 

